Visible light disinfection can be a potent weapon against bacteria in hospital settings
By Clifford J. Yahnke
against bacteria in hospital settings
According to the Centers for Disease Control and Prevention (CDC), approximately one in every 25 U.S. hospital patients contracts an infection in a healthcare setting. This amounts to approximately 1.7 million infections each year with approximately 99,000 of those infections ending in the patient’s death. Battling a Healthcare-Associated Infection (HAI) can often add tens of thousands of dollars to the cost of treating a single patient and can result in significant financial penalties and lower Medicare reimbursements for those healthcare providers who score poorly relative to their peers in this area. For example, the excess cost of a single Surgical Site Infection (SSI) is, on average, $20,785, with much higher costs for complex procedures such as orthopedic joint replacements.1
With the discovery of penicillin in 1928, the medical community was given a powerful and easy-toadminister weapon against infections beginning in 1942. However, this weapon has proven to be a double-edged sword, as over time, it has triggered an adaptation response in infection-causing organisms, leading to strains that are now resistant to most (or all) forms of antibiotics. Says Dr. Arjun Srinivasan, an associate director for the Centers for Disease Control and Prevention, “We have reached the end of antibiotics, period.”
As our ability to treat infections decreases, there is an increased need to preemptively prevent bacteria from entering the body. In fact, infection prevention has become so important that many healthcare providers now have one or more full-time, certified professionals to oversee their efforts in this area.
Within the field of infection prevention, there are several subspecialties related to different types of infections, medical procedures and clinical settings. There is also another specialty called “environmental disinfection” that focuses on the role of pathogen transmission through contaminated air and surfaces. While improved handwashing remains one of the most effective ways to reduce the transfer of pathogens, there are numerous studies demonstrating that bacteria and viruses can survive on surfaces for up to 12 months, and that these same organisms can make their way from those surfaces into patients, causing serious infections.2, 3, 4
LEDs AS GERMACIDE
LED technology affords the luminaire manufacturer the opportunity to more efficiently create highly customized spectra that provide a range of non-visual benefits for applications such as horticulture and healthcare. One healthcare application, which has garnered less public attention to date but can have far-reaching benefits, is visible light environmental disinfection.
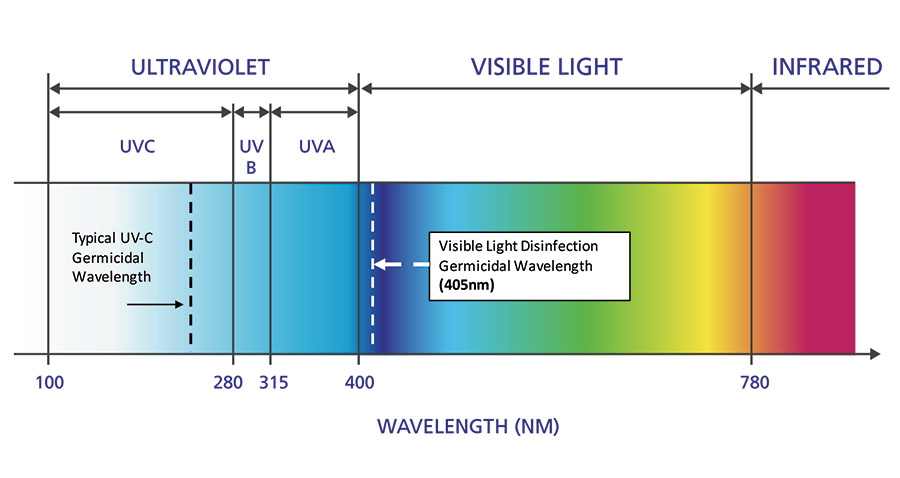
Sunlight has been used throughout the course of history to kill bacteria in various settings.5, 6 This phenomenon was thought to be largely due to the presence of germicidal ultraviolet (UV) radiation within the solar spectrum. It wasn’t until approximately 15 years ago that researchers at the University of Strathclyde discovered a second disinfecting element within sunlight. Further research by this same group later confirmed that a narrow spectrum of visible, indigo-colored light (405+/-5nm) had a germicidal effect on various medically important bacteria without the need for additional sensitizers.7, 8, 9 The university subsequently created prototype devices wherein the disinfecting spectrum was integrated with overhead lighting to create a whole-room, environmental disinfection device4 (Figure 1). The university was later awarded two different patents for this work and, today, a single manufacturer has commercial authority to create products with this underlying technology.10
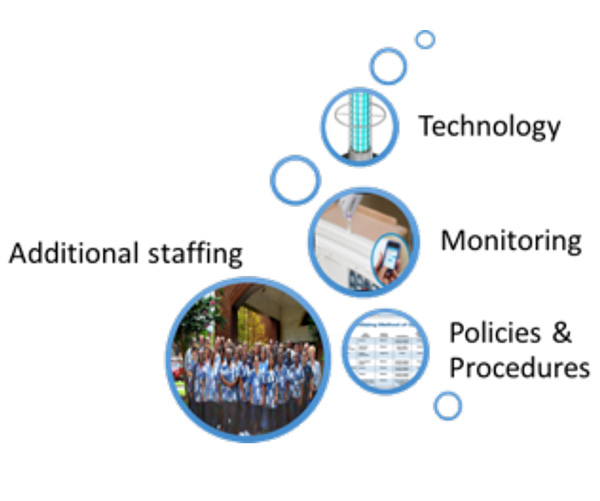

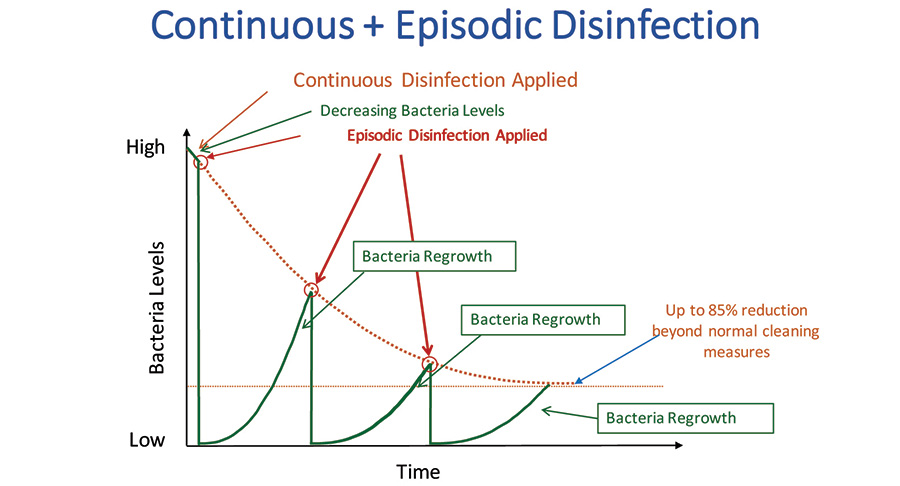
The solution to improving environmental hygiene has typically been a combination of personnel, compliance and technology, as shown in Figure 2. While these efforts are certainly logical, they ultimately reach a point of diminishing return as they require people to implement, thereby making it costly to perform and introducing the potential for human error. As a result, healthcare providers are increasingly searching for solutions that provide a safety net by disinfecting surfaces that may have been insufficiently disinfected. Typically referred to as “whole room disinfection,” such solutions exist to complement or bolster their current efforts. These technologies are commonly segmented by the time over which the disinfection occurs. Most products and technologies are effective for the short period of time over which they are applied, as an extension of regular cleaning protocols. Such efforts are commonly referred to as “episodic.” By comparison, products and technologies that operate over an extended period of time (e.g. HEPA air filters) are referred to as “continuous.” A comparison of episodic versus continuous whole-room disinfection technologies is shown in Figure 3. The benefits of using continuous environmental disinfection, together with normal cleaning protocols, is shown in Figure 4.
VISIBLE LIGHT DISINFECTION
Visible light is an ideal medium for continuous environmental disinfection because virtually every indoor space uses overhead lighting. The visible light scatters from surfaces, allowing it to fill the room and provide a ubiquitous disinfection effect.
At the same time, integration of this disinfecting element into the room’s overhead lighting requires a careful consideration of the underlying visual needs of the room’s users and their occupancy patterns. For example, an operating room has a large amount of ambient white light (200-300 footcandles near its center) and is in use for roughly 12 hours per day. This defines the amount of disinfecting light that can be introduced into the room without distorting visual acuity. Since the room is only in use for 12 hours per day, an alternative mode of operation—using indigo light only—provides substantially higher levels of disinfection, leaving the room in a cleaner state for the start of the next day.
The last consideration is the number of fixtures needed, per room, to create clinically relevant disinfection. This is a complex topic that subtly affects the fixture design, as one must balance several considerations:
- The need for sufficient, but not excessive, amounts of white light
- The need for sufficient disinfection
- The need for the white light to provide desired color rendering (CRI) and color quality (Duv)
- The need to minimize the ceiling footprint; ideally limiting the technology to a 1:1 replacement for standard ambient light fixtures
Ultimately, these trade-offs are underpinned by an understanding of the clinical, rather than laboratory, performance of the product; with the key differences being the varying light levels within the room throughout the day, the environmental conditions affecting the bacteria and the continuous reintroduction of bacteria into the environment by people within the space.
EARLY INTERVENTION
With increasing public awareness of the growing superbug threat, building owners will look to use every tool at their disposal to reduce HAIs, including the building itself. Visible light disinfection is an emerging lighting application providing non-visual benefits that align with this goal, resulting in products that offer an ROI of less than one year. It’s up to lighting professionals to introduce the technology to their customers at the earliest opportunity.
This article was adapted from a presentation delivered at LEDucation 11.

